Developmental Kyphosis
Hyperkyphosis (forward bend of the thoracic [ribbed] vertebrae beyond normal limits) is classified as either postural or structural in origin.
Postural Kyphosis
Postural kyphosis is flexible and will correct when the patient is asked to stand up straight. Patients with postural kyphosis have no abnormalities in their vertebrae shape.
Structural Kyphosis
Structural kyphosis, known as Scheuermann's kyphosis, is defined as rigid. The front sections of the vertebrae grow slower than the back sections. The abnormal kyphosis is best viewed from the side in the forward-bending position where a sharp, angular abnormal kyphosis is clearly visible.
Instead of normal, rectangular vertebrae with ideal alignment, wedge-shaped vertebrae cause misalignment (Figures 1 and 2). This process occurs during a period of rapid bone growth (usually between the ages of 12 and 15 in males or a few years earlier in females). The kyphotic curve that develops with growth frequently remains mild and requires only periodic x-rays.
Patients often have poor posture and complaints of back pain, which is most common in early teenage years and less so as they approach adulthood. The pain rarely interferes with daily activity or professional careers. The kyphosis is more likely to be painful the apex (most angular section) is in the mid-to-low back instead of the upper back. In severe cases, adolescents may not be able to lie on their back without several pillows under their head.
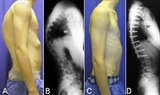
A) Preoperative photo of patient with severe kyphosis secondary to Scheuermann's disease. B) Preoperative x-ray of the same patient. C) Postoperative photos of the same patient one year after surgical correction of the kyphosis. D) Postoperative x-ray of the same patient
Treatments
Observation
The behavior of the curve may be monitored via repeated clinic visits and x-ray examinations at various times during development for worsening or progression of the scoliosis.
Bracing
Bracing or casting programs may help by allowing growth while minimizing increases in the scoliosis. The need for surgery may be delayed and, in some instances, avoided.
Surgery
Surgery is generally recommended if brace or cast treatment should fail to keep the scoliosis from progressing, or if the curve pattern does not appear amenable to brace or cast treatment.
