Coding & Reimbursement
This page is the center for your coding issues and answers with regard to spinal deformity. In the Coding Article Archive you can find all Coding Committee articles from the SRS Member Newsletter. Topics discussed range from correction to ICD-10. Our next section of the page, our current project, will provide examples of common coding scenarios for you to reference. Lastly, if you have any questions, please browse our FAQs page. Still can't find the answer? You can also submit a question on that page and see the answer posted to the FAQs shortly afterward.
Coding Article Archive
Complications of Spine Surgery in ICD-10
Complications of Spine Surgery in ICD-10
March 2018: R. Dale Blasier, MD, FRCS(C), MBA
The ICD-10 tabular list of codes offers great granularity and variety in the description of complications which may occur associated with spinal surgery. The ICD-10 codes were initially developed for epidemiology but now have developed into a major mechanism for documenting medical necessity for medical or surgical treatment. Payers routinely consider ICD-10 codes in determining payment decisions for treatment of post-op complications.
Complication codes fall into several categories, these include:
- Generic complications of any surgery
- Complications after musculoskeletal procedures
- Intraoperative and post procedural complications and disorders of musculoskeletal system
- Intraoperative and postprocedural complications and disorders of nervous system
- Other surgical complications
It is worthwhile to look at these complications, and where they reside within the ICD-10 codeset.
Generic complications of any surgery during or after a procedure are listed in T81-T86.
Because these are listed in the T-section – these are considered injuries and require a 7th digit (usually “A”). The seventh digit “A” should be appended if the complication is under active treatment. The seventh digit “B” should be appended if the complication is healing routinely. The seventh digit “S” should be appended indicating a sequela or late effect of a complication. These complications include:
- Shock T81.1
- Disruption of external surgical wound T81.31X (i.e. dehiscence of skin)
- Disruption of internal surgical wound T81.32X (i.e. dehiscence of fascia)
- Infection T81.4XX. This covers a wide variety of possibilities:
- Intra-abdominal abscess following a procedure
- Postprocedural infection, not elsewhere classified
- Sepsis following a procedure
- Stitch abscess following a procedure
- Subphrenic abscess following a procedure
- Wound abscess following a procedure
- Retained foreign body T81.500 (i.e. instrument, sponge, unattached implant)
- Vascular injury T81.7
- Breakdown (mechanical) of internal fixation device of vertebrae T84.216
- Breakdown (mechanical) of internal fixation device of other bones T84.218
- Breakdown (mechanical) of other internal orthopedic devices, implants and grafts T84.418
- Displacement of other internal orthopedic devices, implants and grafts T84.42
- Infection and inflammatory reaction due to internal fixation device of spine T84.63
- Complications of bone graft T86.83. There are several possibilities:
- T86.830 Bone graft rejection
- T86.831 Bone graft failure
- T86.832 Bone graft infection (Use an additional code to specify type of infection)
- Infection and inflammatory reaction due to other internal orthopedic prosthetic devices, implants and grafts T84.7
- Pain due to internal orthopedic prosthetic devices, implants and grafts T84.84
Complications after musculoskeletal procedure M96.0 – M96.6
These probably should be labelled “complications after spine treatment”, but they are not. These are listed in the M chapter and are considered diseases and do not require a seven digit. These include:
- Pseudarthrosis after fusion or arthrodesis M96.0
- Post laminectomy syndrome M96.1
- Post radiation kyphosis M96.2
- Post laminectomy kyphosis M96.3
- Postsurgical lordosis M96.4
- Post radiation scoliosis M96.5
- Fracture of bone following insertion of orthopedic implant, prosthesis or bone plate M96.6
Intraoperative and post procedural complications and disorders of musculoskeletal system, not elsewhere classified M98.6
These complications describe injury to a musculoskeletal structure which result from a procedure which may or may not be musculoskeletal in nature.
- Intraoperative hemorrhage and hematoma of a musculoskeletal structure M96.81
- Accidental puncture and laceration of a musculoskeletal structure M96.82
- Post procedural hemorrhage of a musculoskeletal structure M96.83
- Post procedural hematoma or seroma of a musculoskeletal structure M96.84
- Postprocedural hematoma of a musculoskeletal structure following a musculoskeletal system procedure M96.840
- Postprocedural hematoma of a musculoskeletal structure following other procedure M96.841
- Postprocedural seroma of a musculoskeletal structure following other procedure M96.842
Intraoperative and postprocedural complications and disorders of nervous system, not elsewhere classified G97
These are found in the G chapter. They are considered diseases and not injuries.
- CSF leak from spinal puncture G97.0
- other reactions to spinal lumbar puncture including headache G97.1
- intraoperative hemorrhage and hematoma of a CNS structure complicating a procedure G97.3
- intraoperative hemorrhage and hematoma of a CNS structure following a CNS procedure G97.31
- intraoperative hemorrhage and hematoma of a CNS structure following other procedure G97.32
- inadvertent durotomy during a procedure G97.41
- puncture of other CNS organ during a CNS procedure G97.48
- puncture of other CNS organ during other procedure G97.49
- Postprocedural hemorrhage and hematoma of a nervous system organ or structure following a nervous system procedure G97.51
- Postprocedural hemorrhage and hematoma of a nervous system organ or structure following other procedure G97.52
- Other intraoperative procedural complications of the nervous system G97.81
- Other postprocedural complications of the nervous system G97.81
Other surgical complications:
- Acute blood loss anemia D62
- Ileus K56.7
- Acute embolism and thrombosis of unspecified deep veins of lower extremity (specific to involved vein) I82.40 (i.e. VTE. Codes differ according to which vein is involved)
- Urinary retention R33.9
There is a wide variety of conditions described in ICD-10 which can be used to document post-op complications of spine surgery. They are not all described in this article. Often the language used to describe these conditions is not obvious, so it is hoped that exposure to the language of the conditions in this article will aid in the search for the correct ICD-10 code.
Return to TopCoding Posterior Interbody Fusion with Decompression (the Byzantine world of medical coding)
Coding Posterior Interbody Fusion with Decompression (the Byzantine world of medical coding)
September 2017: Matthew D. Hepler, MD
One of the most frequent coding controversies over the last several years has been how to properly code a posterior interbody fusion (22630 or 22633) with a decompression (laminectomy/63047) at the same level. This is an important issue as lumbar interbody fusions and decompressions are some of the most common spine procedures performed and improper coding can lead to CMS audits. More interestingly, exploring this “coding conundrum” in detail helps unveil some of the mechanisms and entities that have come to govern the byzantine process of medical coding.
The primary codes involved include 22630, 22633, and 63047 (for simplicity sake we will not consider some of the add on codes frequently performed in these procedures). The CPT code descriptions are as follows:
22630
Arthrodesis, posterior interbody technique including laminectomy and/or discectomy sufficient to prepare interspace (other than for decompression), single interspace, lumbar.
22633
Arthrodesis, combined posterior or posterolateral technique with posterior interbody technique including laminectomy and/or discectomy sufficient to prepare interspace (other than for decompression), single interspace, lumbar.
63047
Laminectomy, facetectomy, and foraminotomy (unilateral or bilateral) with decompression of spinal cord, equine, and/or nerve root(s) (eg spinal or lateral recess stenosis) single vertebral segment, lumbar.
CPT Guidelines
One of the first distinctions to recognize is that arthrodesis codes are in the Musculoskeletal System chapter of CPT (22590-22634) and posterior decompression codes are in the Nervous System section of CPT (63001-63066). These are different organ systems and CPT has, logically, always maintained it is appropriate to include the additional code for a decompression when performed at the same level as a fusion, even though it may be through the same incision. So for example a spondylolisthesis with severe stenosis may be treated with a postero-lateral fusion (22612) and a laminectomy (63047-51). Remember stand alone codes include the work for the 90 day global period as well as the intra operative work; modifier 51 (multiple procedures) allows additional stand alone procedures which are “discounted” to appropriately represent the additional intra operative work involved (the work RVUs for the 90 day global already accounted for by the first, highest RVU valued primary code).
This is simple enough in the above example when the primary procedures involve distinctly different organ systems. The posterior interbody codes (22630 and 22633) are more complicated because they require some degree of decompression/laminectomy to perform the interbody fusion even though the original vignette used to create the code was for a revision fusion procedure with minimal signs of nerve root dysfunction. Attempts were made to clarify this distinction early on with the CPT editorial change: “laminectomy and/or discectomy sufficient to prepare the interspace (other than for decompression).
So for example a patient undergoing a posterior interbody fusion with leg pain due to lateral recess stenosis/HNP would not justify the additional laminectomy code since the work involved in removing portions of the lamina, facet and disc are included in the interbody procedure. This is also the case when the stenosis is contralateral to a single sided TLIF approach since the vignette for the posterior interbody codes includes a bilateral approach (the vignette is the specific clinical scenario used to create a new code).
However, CPT guidelines clearly state that additional decompression beyond the necessary laminectomy, facetectomy, or discectomy to access the interspace may be separately reported. So for example a patient undergoing an interbody fusion with severe canal and/or foraminal stenosis who requires a complete laminectomy for decompression beyond what is necessary to prepare the interbody space for fusion would report 22630/22633 with 63047. This might include modifier 51 multiple procedures or modifier 59, distinct procedural service (more on this later). You must, of course, provide adequate documentation in the operative report supporting the need for and performance of any such distinct or additional procedures.
Medicare Guidelines (the Byzantine twist)
Although CPT guidelines clearly state that additional decompression beyond that necessary to prepare the disc space may be reported separately (and many payors follow these CPT rules), CMS has disregarded them and prohibited payment for 63047 with 22630/22633 at the same level since 2015. To understand how we arrived at this conflicting set of guidelines we have to examine how CMS adopted the use of CPT codes (which are owned and maintained by the AMA) while developing its own software (NCCI) to regulate their use (see Modifer 59 SRS newsletter August 2016).
NCCI (National Correct Coding Initiative), CMS’s national editing software system, was developed in the 1990s to detect and prevent “unbundling (billing multiple procedure codes when one code is more appropriate). These NCCI edits apply only to services that are performed on the same day, for the same patient, and billed by the same physician. These edits identify an exhaustive list of code pair combinations that generally should not be reported together by a provider on the same day of service. They further specify combinations which should: never be reported together (0), that may be reported together in special circumstances with an appropriate modifier (1), or are mutually exclusive (ME). In 1999 the NCCI Policy Manual for Medicare Services implemented edits for code pairs 22630 and 63047, which were updated in 2012 to include 22633 and 63047 and again in 2015. The January 2015 NCCI edit guideline states:
“CMS payment policy does not allow separate payment for CPT codes 63042 (laminotomy...; lumbar) or 63047 (laminectomy...; lumbar) with CPT codes 22630 or 22633 (arthrodesis; lumbar) when performed at the same interspace. If the two procedures are performed at different interspaces, the two codes of an edit pair may be reported with modifier 59 appended to CPT code 63042 or 63047.”
Multiple efforts were made by various spine group coding organizations to resolve the conflict between the CPT and CMS/NCCI guidelines but CMS has elected not to overturn the edit.
More recently, the October 2016 CPT assistant article stated CPT codes 63047 and 22633 may not be reported together at the same interspace. NASS, CNS, AANS, and ISASS wrote an erratum which AMA has denied and efforts to appeal have been unsuccessful to date as there in no appeal process.
In Summary
As noted previously CMS guidelines are in direct conflict with CPT guidelines regarding the combination of posterior interbody fusion with decompression at the same level. As a result coding these procedures has been dependent on the guidelines of the specific payer.
For Medicare/Medicaid (CMS) you may code for 22630/22633 with 63047 to document the work performed. CMS will not pay for the decompression (63047) for the reasons explained and this denial should not be repealed. Also, CMS guidelines indicate you should not append a modifier to this coding combination.
Payers that follow CPT guidelines have permirred a laminectomy at the same level as a posterior interbody fusion with appropriate documentation. In these cases it was appropriate to append modifier 59 to indicate a distinct organ system or modifier 51, multiple procedures according to each payers recommendation. More recently, CPT assistant publication states decompression cannot be reported with interbody fusion at the same level; therefore anticipate payers will begin to deny this as well.
Reference:
Laminectomy and Interbody Fusion Confusion.
John Kevin Ratliff, MD, FAANS | Departments | Coding Clarity
AANS Neurosurgeon: Volume 25, Number 1, 2016
Spine Surgery Quandary: Posterior Lumbar Interbody Fusion
When do you bill 63056-59 with 22633, rather than 63047-59?
By Kim Pollock, RN, MBA, CPC, CMDP
AAPC Spine Surgery, June 2016
A Timeline of Posterior Lumbar Interbody Fusion and Decompression of Nerve Roots: Can Posterior Lumbar Interbody Fusion and Decompression Be Reported Together at the Same Interspace?
R. Dale Blasier, MD, Christopher Kauffman, MD, Paul Saiz, MD, NASS Coding Committee
NASS Spineline, April 2016
Are Current Spinal Fusion Hospital Payment Diagnosis Related Groups (DRGS) Adequate?
Are Current Spinal Fusion Hospital Payment Diagnosis Related Groups (DRGS) Adequate?
March 2016: S. Samuel Bederman, MD, PhD, FRCSC and David J. Wright M.Sc.
The SRS Coding Committee, with permission from the Presidential Line, agreed to support an investigation into variation in hospital costs within spinal fusion payment groups to determine whether hospitals are bearing undue financial burden, thus disincentivizing surgeons from performing these important procedures. We report our initial findings from this study.
As rates of spinal surgery have increased, hospital costs have more than tripled, resulting in a significant impact on total U.S. healthcare costs.1–6 Hospital reimbursement from Medicare and other payers to hospitals is provided as a fixed payment for each admission by assigning patients to a Diagnosis Related Group (DRG). Patients are assigned to DRGs according to the principal procedure performed as well as comorbidities or complications managed during the admission.7,8 This system assumes that procedures and patients can be grouped into relatively homogenous units of resource use such that a single payment will adequately cover the costs of hospitalization for most patients within a given DRG.8 However, several factors, including procedural complexity and unique patient characteristics, may contribute to variation within DRGs that lead to differences between hospital costs and payments. Predictable financial losses to hospitals may result in disincentives for the provision of care, potentially leading to disparities in access for some patients by limiting our ability to treat these patients.
Prior work in total hip arthroplasty (THA) revealed that procedural differences, such as those between primary and revision THA, were one source of variation not adequately accounted for in existing DRGs.9 Mean hospital cost, operative time, estimated blood loss, and length of stay were found to be significantly higher for revision THA than for primary THA, even though both procedures were reimbursed equally under a single DRG (DRG 209).9 The cost variation within this DRG, explained largely by procedural differences between primary and revision THA, raised concern for patient access to care as hospitals were deterred from performing revision procedures in an attempt to limit ongoing financial losses.10 Following this study, the Centers for Medicare and Medicaid Services (CMS) effectively “split” this DRG into separate “primary” and “revision” DRGs in an effort to create more homogenous payment groups with more equitable reimbursement. In doing so, the CMS established an effective benchmark for excessive within-DRG cost variation.11,12
A recent study simulating bundled payments in spine surgery suggested that wide cost variation may also exist within current spinal fusion DRGs.13 However, no study has examined current spinal fusion DRGs to determine the magnitude of cost variation within each group. As in total joint arthroplasty (TJA), wide cost variation within spinal fusion DRGs, if present, may lead to discrepancies between hospital costs and payments, placing undue financial burden on some hospitals and potentially compromising access to care for certain patients.
We investigated cost variation within spinal fusion DRGs with a retrospective analysis of the Healthcare Cost and Utilization Project (HCUP) Nationwide Inpatient Sample (NIS) for 2011 which contained over 8 million inpatient admissions from 1,049 hospitals.14
Patients were grouped according to 2011 CMS Medicare Severity-Diagnosis Related Groups (MS-DRGs) and included all patients assigned to spinal fusion DRGs 453 to 460 and TJA DRGs 466 to 470 (Table 1). An aggregate of TJA DRGs 466 through 470 were used to re-create “DRG 209,” which served as a benchmark for cost variation in this study. We measured variation using the coefficient of variation (CV), defined as the ratio of the standard deviation (SD) to the mean (CV=SD/mean x 100), for all direct hospital costs within each DRG.15–17
Table 1. Medical Severity-Diagnosis Related Groups included in this study.
| DRG | Title |
| 209† | Maj Joint/Limb Reattach Procs of Low Extremity (TJA2005) |
| 453 | Combined anterior/posterior spinal fusion with MCC (APF+MCC) |
| 454 | Combined anterior/posterior spinal fusion with CC (APF+CC) |
| 455 | Combined anterior/posterior spinal fusion without CC or MCC (APF) |
| 456 | Spinal fus exc cerv w spinal curv/malig/infec or 9+ fus with MCC (CF+MCC) |
| 457 | Spinal fus exc cerv w spinal curv/malig/infec or 9+ fus with CC (CF+CC) |
| 458 | Spinal fus exc cerv w spinal curv/malig/infec or 9+ fus without CC or MCC (CF) |
| 459 | Spinal fusion except cervical with MCC (SF+MCC) |
| 460 | Spinal fusion except cervical without CC or MCC (SF) |
| 466 | Revision of Hip or Knee Replacement with MCC (RTJA+MCC) |
| 467 | Revision of Hip or Knee Replacement with CC (RTJA+CC) |
| 468 | Revision of Hip or Knee Replacement without CC or MCC (RTJA) |
| 469 | Major Joint Replacement or Reattachment of Lower Extremity with MCC (TJA+MCC) |
| 470 | Major Joint Replacement or Reattachment of Lower Extremity without CC or MCC (TJA) |
† DRG 209 only existed prior to 2004. For this study, DRG 209 was reconstructed by combining all current TJA DRGs back into one DRG. APF = “anterior/posterior fusion” (combined anterior/posterior spinal fusion). CF = “complex fusion” (spinal fusion except cervical with spinal curvature, malignancy, infection or 9+ fusion levels). SF = “spinal fusion” (spinal fusion except cervical). MCC = Major Complication or Comorbidity. CC = Complication or Comorbidity.
Variation (measured by CV) in cost within spinal fusion DRGs ranged from 44.2 for DRG 460 (Simple Fusion) to 52.6 for DRG 456 (Complex Fusion with Major Comorbidity/Complication). The benchmark group, DRG 209 (TJA2005), had a CV of only 38.2. When compared to this benchmark, all spinal fusion DRGs had significantly higher CVs (p-values < 0.0001). The mean costs for spinal fusion DRGs ranged from $27,153 for DRG 460 to $77,965 for DRG 456 while the estimated cost for TJA DRG 209 was only $15,903. In general, the cost variation as well as costs increased with increasing procedural and patient complexity (Figure 1).
Figure 1. CVs for DRGs grouped by procedural category and medical severity.
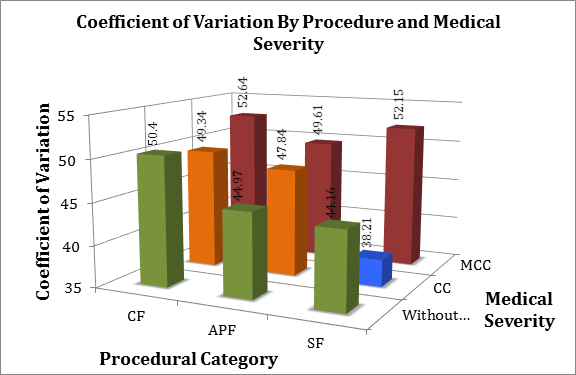
DRGs grouped by procedural category (x-axis) and medical severity (z-axis). CV is plotted on the y-axis. The control TJA DRG is highlighted in blue. CF = “complex fusion” (spinal fusion except cervical with spinal curvature, malignancy, infection or 9+ fusion levels). SF = “spinal fusion” (spinal fusion except cervical). MCC = Major Complication or Comorbidity. CC = Complication or Comorbidity. Without = without MCC or CC. Note that SF does not have a “CC” DRG in the 2011 MS-DRG coding.
As in TJA, procedural factors such as surgical approach, invasiveness, and complexity are sources of cost variation within spinal fusion DRGs that may serve as potential targets for coding changes that could be implemented to further homogenize spinal fusion payment groups. While it could be argued that procedural factors are already accounted for by procedural categories in current spinal fusion DRGs, this study demonstrates that current categories do not, in fact, define homogenous units of resource use, suggesting that reevaluation is warranted.
To further illustrate why there may be significant variation in current DRGs, consider a “standard fusion” (spinal fusion except cervical) procedural category (DRGs 459 and 460). This category makes no distinction between an eight-level fusion and a one-level fusion as long as both procedures are performed from a single (e.g. posterior) approach and do not involve curvatures, malignancies, or infections. Furthermore, even seemingly common procedures such as a single level fusion can have a wide range of outcomes based on procedural factors that are not captured in current DRGs. For example, in a study of patients undergoing one-level or two-level transforaminal lumbar interbody fusion (TLIF), hospital length of stay varied from 3 days for patients who received a minimally invasive TLIF to 4.2 days for those who received a traditional open TLIF.18 The increased length of stay associated with a traditional open TLIF might significantly increase total hospital costs. However, the current DRGs for single-level posterior fusion (DRG 459 or 460) make no distinction between these surgical approaches. Unlike TJA DRG 209, which could be re-categorized into separate DRGs based on clearly defined “primary” and “revision” procedural factors, it may not be feasible to categorize spinal fusion DRGs in a similar fashion given the multitude of different procedures utilized. Rather, it may be more appropriate to explore other procedural measures, such as the degree of surgical invasiveness, to more accurately define homogenous payment groups.19
In summary, this preliminary analysis demonstrates that current cost variation within spinal fusion DRGs is excessively high. Both patient medical severity (complications and comorbidities) and procedural factors (approach, invasiveness, complexity) appear to contribute to the high degree of cost variation within groups. As previously demonstrated in TJA aggregate DRG 209, this variation may be leading to differences between hospital costs and payments that places undue burden on some hospitals and potentially compromises access to care for patients.10 This study highlights the need for future work to identify potential changes in coding for current spinal fusion payment groups. By grouping patients into more homogenous units of resource use, a single fixed payment would more adequately cover the costs of hospitalization for patients within each group. In an atmosphere of healthcare reimbursement that is rapidly moving towards episode-based bundled payments, such efforts to homogenize payment groups will ensure equitable hospital reimbursement and improved patient access to care.
References
- Rajaee, S. S., Bae, H. W., Kanim, L. E. a & Delamarter, R. B. Spinal fusion in the United States: analysis of trends from 1998 to 2008. Spine (Phila. Pa. 1976). 37, 67–76 (2012).
- Baaj, A. A., Downes, K., Vaccaro, A. R., Uribe, J. S. & Vale, F. L. Trends in the treatment of lumbar spine fractures in the United States: a socioeconomics perspective. Journal of Neurosurgery: Spine 15, 367–370 (2011).
- Weinstein, J. N., Lurie, J. D., Olson, P. R., Bronner, K. K. & Fisher, E. S. United States’ trends and regional variations in lumbar spine surgery: 1992-2003. Spine (Phila. Pa. 1976). 31, 2707–2714 (2006).
- Deyo, R. A. et al. Trends, major medical complications, and charges associated with surgery for lumbar spinal stenosis in older adults. JAMA 303, 1259–1265 (2010).
- Cowan, J. A. et al. Changes in the utilization of spinal fusion in the United States. Neurosurgery 59, 15–20; discussion 15–20 (2006).
- Cherkin, D. C., Deyo, R. A., Loeser, J. D., Bush, T. & Waddell, G. An international comparison of back surgery rates. Spine (Phila. Pa. 1976). 19, 1201–1206 (1994).
- Centers for Medicare and Medicaid Services. Acute Inpatient PPS. (2014). at
- Hsiao, W. C., Sapolsky, H. M., Dunn, D. L. & Weiner, S. L. Lessons of the New Jersey DRG payment system. Health Aff. (Millwood). 5, 32–45 (1986).
- Bozic, K. J. et al. Hospital resource utilization for primary and revision total hip arthroplasty. J. Bone Joint Surg. Am. 87, 570–576 (2005).
- Barrack, R. L. The evolving cost spectrum of revision hip arthroplasty. Orthopedics 22, 865–6 (1999).
- Bozic, K. J. CMS changes ICD-9 and DRG codes for revision TJA. AAOS Bulletin (2005). at
- Centers for Medicare and Medicaid Services. Medicare Program; Changes to the Hospital Inpatient Prospective Payment Systems and Fiscal Year 2006 Rates. Federal Register Vol. 70, No. 155 47303–47305 (2005). at
- Ugiliweneza, B. et al. Spinal surgery: variations in health care costs and implications for episode-based bundled payments. Spine (Phila. Pa. 1976). 39, 1235–42 (2014).
- Healthcare Cost and Utilization Project (HCUP). Overview of the National (Nationwide) Inpatient Sample (NIS). Agency for Healthcare Research and Quality (2015). at
- Reed, G. F., Lynn, F. & Meade, B. D. Use of coefficient of variation in assessing variability of quantitative assays. Clin. Diagn. Lab. Immunol. 9, 1235–9 (2002).
- Pope, G. C., Welch, W. P., Zuckerman, S. & Henderson, M. G. Cost of practice and geographic variation in Medicare fees. Health Aff. 8, 117–128 (1989).
- Luft, H. S. Economic incentives to promote innovation in healthcare delivery. Clin. Orthop. Relat. Res. 467, 2497–505 (2009).
- Villavicencio, A. T., Burneikiene, S., Roeca, C. M., Nelson, E. L. & Mason, A. Minimally invasive versus open transforaminal lumbar interbody fusion. Surg. Neurol. Int. 1, 12 (2010).
- Mirza, S. K. et al. Development of an index to characterize the ‘invasiveness’ of spine surgery: validation by comparison to blood loss and operative time. Spine (Phila. Pa. 1976). 33, 2651–2661; discussion 2662 (2008).
Preparing for Conversion to ICD-10
Preparing for Conversion to ICD-10
September 2015: R. Dale Blasier, MD
Preparing for conversion to ICD-10 will require some effort on behalf of each physician and his or her support staff. This will require changes in instrumentation, software, billing forms, training and the way we document patient care. It can’t become “cold turkey,” there must be some advanced planning.
On October 1, 2015, ICD-10 will be switched on for Part A and B of Medicare and almost all private payers. ICD-9 will be switched off as the HIPAA/CMS standard. Use of ICD-9 will result in payment denials. There will be no impact on usage of Current Procedural Terminology (CPT codes) or Healthcare Common Procedures Coding System (HCPCS) codes. CPT and HCPCS Level II and III codes will continue to be used for physician and ambulatory services including physician visits to inpatients and for supplies.
The new code set differs from ICD-9 in many ways. ICD-9 had around 14,000 diagnosis codes. ICD-10 has around 69,000 codes and many of these are musculoskeletal. ICD-9 codes consist of three to five digits maximum and include no placeholders. ICD-10 codes consist of three to seven digits or number and incorporate “X” as a place holder at the 5th and 6th positions to make sure the important fields are always filled. In ICD-9, it was not possible to specify laterality. ICD-10 there are codes to specify right, left or bilateral for most conditions. In ICD-9, fractures could be specified as open or closed. In ICD-10 they can be specified as open or closed and the degree of open fracture using the Gustilo classification. In ICD-10 there is extensive use of combination codes – for instance, osteoporosis with fracture.
For the description of injury, ICD-9 codes were arranged by type of injury. Within ICD-10, injuries are grouped by anatomic site.
In ICD-10, there are 21 chapters, which describe just about every injury or malady known to man. For spinal deformity surgeons, the chapters most relevant are Chapter 6 – The Nervous System; Chapter 13 – The Musculoskeletal System and Connective Tissue; Chapter 17 – Congenital Malformations, Deformations and Chromosomal Abnormalities; and Chapter 19 – Injury, Poisoning and Certain other Consequences of External Cause.
Most diagnoses relevant to spine surgery will reside in Chapter 13 under Diseases of the Musculoskeletal System. Almost every condition that ends with “-itis” or “-osis” will be found here such as scoliosis, kyphosis, lordosis, spondylosis, osteoporosis, etc. Similarly codes for osteomyelitis, discitis, arthritis and myositis and the like will be found here.
Traumatic conditions reside in Chapter 19 – the injuries section. There they are listed by body part, starting at the head and working downward. They include fractures and dislocations, sprains and strains, wounds, burns and other things including some surgical complications.
Many of the conditions we treat are not described in the same language we would use day to day in our practices. For this reason, it imperative for physicians to look for the diagnoses which they commonly use to see how they are described within ICD-10. This will make it easier to find similar codes in the future by using the correct language. For instance, “post thoracotomy scoliosis” would be described by “other secondary scoliosis”. Users will also find much more granularity and specificity of codes with ICD-10. In ICD-9, idiopathic scoliosis in all ages and regions of the spine were described by one code – 737.30; In ICD-10 there are multiple codes for scoliosis sorted by age (0-4 years, 5-10 years, 11-17 years and 18 or greater years) and location of the scoliosis within the spine (cervical, cervicothoracic, thoracic, thoracolumbar, lumbar, lumbosacral). In order to specify the correct ICD-10 code the physician will need to document age and curve location for each patient.
New to ICD-10 is the seventh character or extension field. This field is relevant to injuries and not so much for diseases. It specifies information about encounter type (initial, subsequent, or sequela), type of fracture healing (routine, delayed, nonunion, or malunion) and openness of fracture (Gustilo I or II or Gustilo IIIA, IIIB, or IIIC). The seventh digit will not be utilized for deformities or diseases of spine. They will only be relevant in cases of trauma (fracture or dislocations) found in the injury chapter and insufficiency fractures of the spine found in the diseases chapter.
There has been considerable interest in the lay press about codes in ICD-10 for external causes of morbidity – for instance “injured while on burning water skis”. However, there is no national requirement for us to provide these codes regarding the external cause.
The challenge for the spinal deformity surgeon in the adoption of ICD-10 will be the requirement for increased documentation. More information will need to be obtained from the patient and documented in the medical record to arrive at the new and specific diagnoses in ICD-10. This will take more time than in the past and unfortunately, there is no increased compensation for the increased time. It will be difficult for the deformity surgeon to document relevant co-morbidities because while the spine surgeon is well-versed in orthopaedic and spinal diagnoses, he or she is less-well familiar with documentation of medical conditions which may affect healing or outcome – such as heart disease, smoking, diabetes, hypertension, obesity and the like. We will need to learn to document these for risk stratification. It will be important in the future to indicate which cases are “the hard ones” and should be compensated as such. How is it possible to pick out codes for the relevant commorbidities? The choices include: ask the patient and look up each code; import codes from the EHR; obtain them from the referring physician; or use unspecified codes. This could take considerable time and practice to “get it right”.
How is it possible to find the correct code for each patient? While it would seem intuitive for the surgeon to make a list of existing ICD-9 codes and list the relevant ICD-10 code next to it, practically this doesn’t work because a single ICD-9 code may correspond to dozens of ICD-10 codes. As a result, physicians look to Generalized Equivalence Mappings (GEMS), cheat sheets, books, software, and the Internet. GEMs work to map existing ICD-9 codes to regions of ICD-10 where similar diagnosis types may be found. Cheat sheets are usually one-page, highly specialized condensations of a larger GEM. Many cross reference books are available from the AMA and coding associations. Program such as Code-X developed by the AAOS have extensive search functions which can lead to a correct code with a minimum of keystrokes. When in doubt – just Google it. Many sites such as ICD-10 Data.Com are helpful and free.
The main take-home message is that is imperative for the physician to look at ICD-10 before October 1st and see how the codes are described and what documentation will be required to lead to the correct code.
Download ICD-10 Cheat Sheet (PDF)
Return to TopRelative Value Units (RVUs); Definition and Applications
Relative Value Units (RVUs); Definition and Applications
March 2015 Newsletter: Shay Bess, MD
The working relationship between physicians, hospitals and university health care systems has expanded with an increased number of physician employment agreements. Traditionally physician employments, either through a university, a hospital or a health care system, have been based upon a fixed salary. More recently, an increased emphasis has been placed upon incentive based physician employment contracts that are dependent upon physician productivity. Often physician productivity is assessed by reimbursements or “collections” from the physician’s clinical/surgical practice, however, use of collections as a gauge for physician productivity may be inaccurate, because many of the collection dollars are dependent upon payer mix and/or the diligence of the collection agency. Consequently, the “collections” might not be truly reflective of the physician work that is being done. Relative value units (RVUs) and work RVUs (wRVUs) may provide a more accurate assessment of physician productivity. The purpose of this article is to provide an overview of the definition and function of RVUs and wRVUs so that physicians reading this article can gain a better understanding of how RVUs 1) affect reimbursements, 2) provide a more accurate assessment of clinical work that is being done, and 3) provide knowledge foundation to help physicians negotiate with their work place.
RVUs are numeric values that are ascribed to services provided by physicians, health care assistants and the health care institution that were created to provide a standardized measure of value for all health care services. The RVU system is part of the resource-based relative value scale (RBRVS) that is a government based effort to create a standardized reimbursement formula to help direct health care services reimbursement. This standardized reimbursement formula, in turn, generates the dollar benchmark for service reimbursement by using Medicare reimbursement dollars as a gauge to guide payment. For the Medicare system, the RVUs for a particular service are multiplied by a dollar conversion factor. The Medicare dollar value is then established as the reference point for reimbursements of services, and then, accordingly, other payers such as Medicaid and private payers pay for services as per their reference to the Medicare benchmark standard. Medicaid on average reimburses approximately 70 percent of Medicare values, whereas third party payers typically pay 130 percent of Medicare or more, based upon institutional contracts, state fee schedules and if the providing physician is in or out of network for the third party payer (more information on Medicaid and Medicare fee schedules is provided on several websites including www.kff.org: state health facts, and www.cms.gov). The Medicare fee schedule currently encodes over 7,500 physician services that are based upon Current Procedural Terminology (CPT) codes. The dollar amounts for these CPT codes are posted online www.gpo.gov/fdsys/ as well as on the RVU Wikipedia page under the federal register link. For each service or procedure, Medicare determines three different subtypes of RVUs; physician work RVUs, practice expense RVUs and professional liability insurance RVUs.
Physician work RVUs (wRVUs) attempt to account for the time and effort required for a service and, if the service is surgical, the wRVUs also attempt to account for the work involved during the 90-day global period for post-procedural follow up. Practice expense RVUs were created to account for the nonphysician clinical and nonclinical labor and institutional expenses that encompass the designated service. Professional liability insurance RVUs attempt to account for the cost of malpractice insurance for the physician/service. The formula for calculating the Medicare fee schedule payment amount for a given service is:
Payment = [(RVU work x geographic practice cost indices work) + (RVU practice expense x geographic practice cost indices practice expense) + (RVU Malpractice x geographic practice cost indices Malpractice)] x conversion factor
In this payment formula, “geographic practice cost indices” factor the geographic differences of the cost of clinical practice across the country, and the “conversion factor” is a dollar multiplier that is updated on an annual basis according to a formula specified by government statute. In 2014, the conversion factor was $35.8228, and the conversion factor for January 1, 2015, through March 31, 2015 is $35.7547. The definition and numeric value in wRVUs ascribed to each service initially came from a series of Harvard based studies in the late 1980s in which physicians were asked to estimate the amount of work involved for different medical services based on medical vignettes and a subsequent consensus was reached for the specific number of wRVUs assigned for a service. The number of wRVUs (and total RVUs) for each specific service, as well as RVUs for new services, are updated at minimum every five years through the Center for Medicaid and Medicare (CMS), in conjunction with recommendations from the American Medical Association/Specialty Society Relative Value Scale Update Committee (RUC). The total RVUs and RVU components including wRVUs for a specific service can be calculated on the CMS website by using the Physician Fee Schedule Search Tool, at www.cms.gov/apps/physician-fee-schedule/overview.aspx. Click on Physician Fee Schedule Search Tool and enter the CPT code for a specific service. Using this tool one can easily identify the recommended wRVUs for the following CPT codes;
22843 (posterior segmental instrumentation 7-12 segments) = 13.44
22802 (posterior arthrodesis for deformity, 7-12 segments) = 32.11
22633 (posterior lumbar fusion with posterior interbody fusion, one level) = 27.75
63075 (anterior cervical decompression and discectomy, one level) = 19.60
The compensated dollar amount/wRVU is not consistent for all medical specialties. Different specialties are valued differently in compensation potential which is likely a reflection of multiple factors including; potential revenue generated by the specialty, amount of post-graduate required by the specialty, and work hours required by the specialty. The median dollar amounts/wRVU according to each medical specialty are readily available. In 2013, the American Medical Group Association (AMGA) provided the results of a Medical Group Compensation and Financial Survey that polled approximately 280 medical groups representing approximately 67,900 providers. According to the survey results, which provided the 2012 United States median compensation dollar amount per wRVU for multiple medical specialties, the median compensation dollar amount/wRVU for Orthopaedic Surgery providers was $66.63 and the median compensation dollar amount/wRVU for Neurosurgery providers was $71.81. Comparatively, that same year the median compensation dollar amount per wRVU for Family Medicine providers was $42.52.
In summary, an understanding of RVUs and wRVUs can help physicians understand the amount of work that they are doing and their current compensation structure. It is important to understand that RVU values for each service can change according to the recommendations and RVU updates that are provided by the CMS and RUC. Additionally, the conversion factor fluctuates and operative services are often bundled. Therefore, it is recommended that physicians review their RVU and wRVU productivity with their practice managers and/or billing group and reconcile these values with their own case list on a regular basis. This frequent communication and reconciliation can provide greater insight to one’s practice and help guide negotiations for future employment.
Bibliography
- S Coberly. “The Basics; Relative Value Units (RVUs),” National Health Policy Forum, January 12, 2015, www.nhpf.org
- B Vaudrey, S Loos. “CCP Compensation 2013: Evolving Models, Emerging Approaches; Results from the AMGA 2013 Medical Group Compensation and Financial Survey,” Group Practice Journal, September 2013
Are You Ready for ICD-10?
Are You Ready for ICD-10?
September 2014 Newsletter: Christopher J. DeWald, MD
"It was the best of times, it was the worst of times, it was the age of wisdom, it was the age of foolishness, it was the epoch of belief, it was the epoch of incredulity, it was the season of Light, it was the season of Darkness, it was the spring of hope, it was the winter of despair . . ."
Charles Dickens, 1859, in A Tale of Two Cities.
Indeed, Charles Dickens may have been forecasting the coming of the "Age of ICD-10." What is ICD-10? And why are we making such a fuss about it? Is it really the age of wisdom, with informatics and data collection, or is this the age of foolishness that we spend extra time looking at numbers instead of treating patients? Well, we can stay in the winter of despair or look towards a spring of hope and embrace the changes among us.
ICD-10 is the tenth revision of the International Statistical Classification of Diseases and Related Health Problems (ICD). It is a medical classification system endorsed by the World Health Organization (WHO) as the standard diagnostic tool for epidemiology, health management and clinical purposes including morbidity and mortality. It is used to monitor the incidence and prevalence of diseases and health problems to assist in monitoring, treatment and prevention of diseases, allocation of resources and research. ICD-10 was endorsed by the WHO in 1990 and began implementation in member countries as early as 1994. In fact, an ICD-11 revision process has already started and is expected to be released in 2017.
The Best of Times
An ICD system allows for a common language for the countries of the world to share data for the reporting and monitoring of diseases. As electronic medical records become commonplace, the ability to share data is invaluable in helping to shape medical care throughout the world. This is accomplished through ICD. Additionally, the expanded system of ICD-10 will aid the U.S. healthcare system "to measure the quality and safety of (patient) care, process claims for reimbursement and improve clinical, financial and administrative performance." 1
The USA has been using the previous version of ICD, ICD-9, for over thirty years. Most industrialized countries have already made the shift to ICD-10 many years ago. The United Kingdom started using ICD-10 in 1995, Australia in 1998, Russia in 1999 and Canada in 2001. In order to be on par with the world regarding health data, the Center for Medicare and Medicaid Services (CMS) has determined that the U.S. medical field will need to make this change. And it is not just Medicare and Medicaid, third party and private insurance carriers will also follow suit, as HIPAA has mandated that all health insurance companies make the change to ICD-10. Thus, all U.S. physicians and their practices will be affected.
The change to ICD-10 will NOT affect CPT procedural codes that surgeons are well familiar with. ICD codes are assigned to categorize all medical diagnoses and medical conditions for patients. In ICD-10, there is nearly five times the number of diagnosis codes (69,000) compared to ICD-9 (14,000). ICD-10 has three to seven characters instead of only three to five in ICD-9. Most of these changes have occurred in the orthopedic codes including more detail in the anatomic location of disease or injury, the laterality, and much more detail in type of fracture and the subsequent healing of the fracture.
Surgeons will need to know what their coders will be looking for in order to properly code and clearly document this. Coders will need an updated education on anatomy and injury classification systems, such as the Gustilo open fracture classification, to code properly.
The Worst of Times
The worst news is that there will be no grace period. October 1, 2015 is a drop-dead date. All coding after this date will be ICD-10. It has been estimated that there will be a significant drop in productivity and reimbursements after this date for three to nine months due to delay in getting proper documentation and codes, as well as, denials for improper codes. Many professionals have recommended that physician groups take out a line of credit to weather this period in order to keep salaries paid. The Canadian system had a drop of productivity of 33 percent with their change to ICD-10 that took over three years to recover from, and that was with a single payor system.
Although, the start date has been pushed back a couple of times, the current start date is October 1, 2015. But, whether it's this year or next, it is coming down the tracks. In order to prepare ourselves for this change, education is mandatory for just about everyone in your practice. There are numerous resources available including www.cms.gov/ICD10, AAOS and NASS webinars and a live courses such as AAOS sponsored Karen Zupko and associates. It's coming - time to get on board and embrace the "best of times" regarding the improvement in health data collection. Besides, we have no choice.
References:
- Ryan J, Winkelmann J. ICD-10 is Coming-Are You Ready? AAOS Web site.
- Cannon DL, Petrosini AV et al. Make Sure You Get Paid on Oct. 1, 2014 - ICD-10 Readiness. AAOS Webinar series - ICD-10 (part one), Sept. 2013.
- Sullivan W, Blasier D, Kaufman C. ICD-10. NASS Webinar. April, 2013.
- www.cms.gov/ICD10
Posterior Column Osteotomies
Posterior Column Osteotomies
March 2014 Newsletter: Christopher J. DeWald, MD
Posterior spinal osteotomy was initially described in an ankylosed spinal column in 1945 by Smith-Petersen et al. 1 Prior to 2008, the traditional CPT codes used to describe posterior spinal osteotomies were: 22210(Cervical), 22212(Thoracic), 22214(Lumbar), and 22216(additional level). These codes were used to describe any type of posterior spinal osteotomy whether performing a posterior column osteotomy alone or a three-column osteotomy.
In 2008, new CPT codes for three column osteotomies, i.e. pedicle subtraction osteotomy (PSO), 22206(Thoracic), 22207(Lumbar) and 22208(additional level) were added to reflect the additional work involved when performing a three-column osteotomy compared to a single column posterior osteotomy. The additional work involved in a three column osteotomy includes the removal of the entire lamina of the involved vertebrae, ligamentum flavum and partial laminae of the adjacent intervertebral interspaces, resection of the both pedicles, partial resection of the lateral vertebral wall, as well as, the posterior vertebral wall anterior to the cauda equina completely exposing the cauda equina and bilateral nerve roots. 2 The additional work and risk is reflected in a higher RVU value assigned to the three column osteotomy codes. RVU values equate to the surgical procedure, length of surgery, preoperative discussion, risk involved, postoperative inpatient hospital care and the 90-day global postoperative period. Prior to the development of the newer codes being formulated, a surgeon performing a L3 PSO would have had to code his/her procedure as an unlisted code or use the posterior spinal osteotomy code twice (22214 and 22216) to reflect the posterior spinal column resection above and below the pedicle, and add a 22 modifier to describe the additional work to perform a three column osteotomy. Currently, a single 22207 would be used for a L3 PSO.
Despite clarifying and differentiating a PSO from a posterior column osteotomy, there still remains a misunderstanding with the standard posterior spinal column osteotomy. Posterior column osteotomy CPT codes, 22210(Thoracic), 22212 (Thoracic), 22214 (Lumbar), and 22216(additional level) are still used for single column posterior osteotomies. The CPT book describes these codes as being used when a portion(s) of a vertebral segment is cut and removed in preparation for re-aligning the spine as part of a spinal deformity correction. A vertebral segment is described as a complete vertebral bone and its associated articular processes. But, there is more to an osteotomy than simply removing a “portion(s) of a vertebral segment”.
A Smith-Petersen type of osteotomy is described as an “opening wedge osteotomy ”. The procedure and its corresponding code is clearly meant to describe a procedure that develops a gap in the posterior spinal column to allow closure enough to shorten the posterior spinal column and lengthen the anterior spinal column through its disc. Confusion comes from a surgeon performing facetectomies of the inferior facets alone and compressing across the pedicle screws to obtain correction of a spinal deformity. Facetectomies using an osteotome, debridement or burring of the facet joints are considered to be a standard portion of a posterior arthrodesis but it is not consider to be an osteotomy. An osteotomy requires a significant more amount of work then simply removing the inferior facet including the removal of the ligamentum flavum and superior facets bilaterally.
The standard Smith-Petersen Osteotomy (SPO) is most easily understood when the spinal deformity surgeon is performing a posterior column osteotomy in a previously fused or ankylosed spine when the anterior spinal column has not been fused. In this case, the posterior aspect of the spinal column has been fused and must be cut in order to mobilize the spine. A trough is cut through the fusion mass typically starting from the central aspect of the spinal canal and removing bone laterally until a complete gap has been created across the previously fused spine. Ponte described a posterior spinal column osteotomy for thoracic kyphotic deformities. 3 Ponte osteotomies are considered a typical posterior spinal column osteotomy similar to a SPO in the non-fused spine. Ponte described his osteotomy as removing the ligamentum flavum beginning from the midline and proceeding laterally to the facet joints and “continued laterally through the superior articular process of the inferior vertebrae” leaving a gap in the posterior column exposing the neuroforamen bilaterally 3.
Further confusion comes when both decompression and an osteotomy are necessary at the same level. Anatomically, a certain amount of decompression is required when performing an osteotomy and this is reflected within the osteotomy code - the laminectomy is an integral part of a posterior column osteotomy and it is necessary to protect the nerves while correcting the deformity. Thus, a surgeon cannot code for both a decompressive laminectomy and an osteotomy at the same site. If laminectomies are performed at other vertebral segments or levels they are separately reportable requiring a -59 modifier.
Today, Smith-Petersen and Ponte osteotomies are synonymous and used interchangeably. They are usually used to correct a deformity across an unfused interspace/disc space. It is reported to provide 10-15 degrees of correction per interspace/osteotomy performed.
Thus, in coding an adult scoliosis spinal fusion case from T11-S1 with bilateral iliac screws where inferior facetectomies were performed, the proper codes used would be:
- 22802 (multiple level posterior arthrodesis for deformity, 7-12 segments),
- 22843 (posterior segmental spinal instrumentation, 7-12 vertebrae, 8 vertebrae),
- 22848 (Instrumentation into the ilium),
- 20937 (posterior iliac crest bone graft via a separate fascial incision).
Whereas, a degenerative adult hypolordotic scoliosis with limited flexibility with a planned posterior fusion from T11-S1 with iliac screws that requires multiple posterior osteotomies from L1-L5 to obtain lordosis is coded with the posterior osteotomy codes. The posterior column osteotomies, Smith-Petersen or Ponte types, require the complete removal of the intervening ligamentum flavum, and both the inferior and superior facets bilaterally at each osteotomy site. This case example would be coded:
- 22214 (osteotomy of spine, Lumbar), L1-2,
- 22216 x3 (Additional osteotomy level) L2-3, L3-4, L4-5,
- 22802 (multiple level posterior arthrodesis for deformity, 7-12 segments, T11-S1 (7 segments),
- 22843 (posterior segmental spinal instrumentation, 7-12 vertebrae, 8 vertebrae),
- 22848 - (Instrumentation into the ilium),
- 20936- (local bone remove during the same incision from the posterior elements including the spinous processes and bone remaining following the posterior osteotomies).
- Smith-Petersen MN, Larson CB, Aufranc OE. Osteotomy of the spine for correction of flexion deformity in rheumatoid arthritis. J Bone Joint Surg,1945;27: 1-11.
- Bridwell KH, Lewis SJ, Lenke LG, Baldus C, Blanke K. Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance. JBJS A 2003: 85(3):454-463.
- Geck MJ, Macagno A, Ponte A, Shufflebarger HL. The Ponte Procedure: Posterior only treatment of Scheuermann’s kyphosis using segmental posterior shortening and pedicle screw instrumentation. J Spin Dis 2007: 20: 586-593.
Spinal Instrumentation - Coding for Insertion and Removal
Spinal Instrumentation - Coding for Insertion and Removal
September 2013 Newsletter: R. Dale Blasier, MD
There are several CPT Codes which involve removal of hardware. These include:
- 22849 - Reinsertion of spinal fixation device
- 22850 - Removal Posterior non-segmental instrumentation
- 22852 - Removal Segmental posterior instrumentation
- 22855 - Removal Anterior instrumentation
Recently CPT has issued new explanatory language for these codes:
“Codes 22849, 22850, 22852, and 22855 are subject to modifier 51 if reported with other definitive procedure(s), including arthrodesis, decompression, and exploration of fusion. Code 22849 should not be reported in conjunction with 22850, 22852, and 22855 at the same spinal levels.
Only the appropriate insertion code (22840 -22848) should be reported when previously placed spinal instrumentation is being removed or revised during the same session where new instrumentation is inserted at levels including all or part of the previously instrumented segments.
Do not report the reinsertion (22849) or removal (22850, 22852, and 22855) procedures in addition to the insertion of the new instrumentation (22840-22848).”
The guidelines also specify that reinsertion (22849) and/or removal (22850) should not be additionally reported with insertion of new instrumentation (22840-22848). Instead, the intent is that when insertion of instrumentation is performed that involves the original levels as well as new levels, only the appropriate code for the type of instrumentation (anterior or posterior) should be used according to the level(s) of instrumentation performed for the procedure.
In other words:
The removal codes (22850, 22852, and 22855) should be used when taking out hardware is all that is being done and not used when insertion or reinsertion is performed.
The reinsertion code (22849) should be used when hardware is going back in at the same levels/location (i.e. for failed hardware, nonunion, etc.). Reinsertion includes removal (22850, 22852, and 22855).
The insertion codes (22840-22848) are used when new hardware is put in which “exceeds” the previously placed hardware. The insertion codes include removal (22850, 22852, and 22855).
Return to TopThe Initiative to Develop New CPT Codes for VEPTR and Growing Rod Procedures
December 2012 Newsletter: R. Dale Blasier, MD
Many surgeons are performing procedures on the growing spine for Early Onset Scoliosis across the country, which includes VEPTR and growing rod procedures. These procedures, although mature and well-established, do not have their own CPT descriptors. As a result, surgeons have had to choose from existing codes which do not well-describe what is actually done during these procedures.
Because there are no codes which specifically describe these procedures, there are several problems: 1) There are not any standardized description or vignette which applies to these procedures 2) There is not a way to track the number of these procedures done across the country because there is no way to separate growing procedures from standard procedures as they use the same codes 3) It is not possible to track billing and reimbursement for procedures performed on children with early onset scoliosis.
As a result of these problems, the Scoliosis Research Society Coding Committee was tasked with determining whether new codes should be developed which specifically address non-fusion procedures performed on the growing spine. The goals for establishing new codes would be enabling tracking of these procedures, ensuring reimbursement and minimizing denials and to establish correct coding which accurately describes each procedure.
The issue was discussed by the Board of Directors during the 47th Annual Meeting in Chicago, Illinois, USA. It was determined that it would be appropriate to survey the SRS membership to determine satisfaction with the existing codes, determine which CPT codes are being used and assess the level of interest for the development of new codes.
The survey was created and circulated by email to North American members of the SRS in November of 2012. The survey asked if the member performed VEPTR or growing rod procedures and whether they used CPT codes to describe them. Members were asked if they felt they were fairly reimbursed for the procedures. The survey also sought to determine if the member felt there was a need to develop new codes to describe these procedures. Each member was also asked to describe which CPT codes would be used to describe procedures performed during the course of treatment including: 1) insertion, 2) revision, 3) lengthening and 4) removal. The questions were asked for both growing rod and VEPTR procedures.
There was a low rate of response to the survey. Forty three of 61 respondents (71%) used CPT codes to report VEPTR or growing rod procedures. Forty of 59 respondents (68%) favored changing the coding structure for these procedures.
Responses regarding VEPTR procedures:
Thirty two of 63 respondents (51%) performed VEPTR procedures. Only 26% (11 of 42) felt they were fairly reimbursed for their work.
The majority of respondents reported VEPTR insertion procedures using codes for insertion of segmental instrumentation. A smattering of respondents reported insertion of non-segmental instrumentation, unlisted procedures, or did not know what to use. For revision or reinsertion, the majority reported the use of 22849 (reinsertion of hardware) and 22850 (Removal of posterior non-segmental instrumentation). A smattering used an unlisted code or were not sure. For lengthening, almost all used the reinsertion code – 22849. For removal, most reported 22850 (removal of posterior non-segmental instrumentation) or 22852 (removal of posterior segmental instrumentation)
Responses regarding growing rod procedures:
Thirty six of 51 respondents (71%) performed VEPTR procedures. Only 40% (15 of 38) felt they were fairly reimbursed for their work.
The majority of respondents reported growing rod insertion procedures using codes for insertion of segmental instrumentation. A smattering of respondents reported insertion of non-segmental instrumentation, unlisted procedures, or did not know what to use. For revision or reinsertion, the majority reported the use of 22849 (reinsertion of hardware) sometimes with 22850 (removal of posterior non-segmental instrumentation). A smattering used an unlisted code or were not sure. For lengthening, almost all used the reinsertion code, 22849. For removal, most reported 22850 (removal of posterior non-segmental instrumentation) or 22852 (removal of posterior segmental instrumentation).
Problems with utilization of existing codes.
Correct Coding: There are several problems with using existing spinal instrumentation codes: 1) Spinal codes are being used in VEPTR cases in which the hardware does not make contact with the spine. 2) Hardware insertion codes are “add-on” codes and cannot be used in isolation without a “base” code such as arthrodesis. 3) The reinsertion code is being reported, even when no hardware is removed or inserted. 4) There is no agreement among users as to which codes to use. In short, the use of existing codes violates principles of correct coding.
Surgeon satisfaction: Sixty-eight percent of respondents favored changing the coding structure for these procedures. With regard to VEPTR procedures, only 26% of respondents felt they were fairly reimbursed for their work. With regard to growing rod procedures only 40% of respondents felt they were fairly reimbursed for their work.
The Development of new codes
It appears appropriate to proceed with developing a set of codes to describe growing rod and VEPTR procedures for the following reasons:
- The procedures have matured to the point where they merit their own codes sets. Use of existing codes does not accurately describe the procedures.
- Existing codes do not allow tracking of growing procedures in children.
- Surveyed surgeons favor the development of a new code set.
The current plan is to proceed with the development of relevant new codes for these procedures with the assent of the SRS Board of Directors. Member comments for or against this proposal can be sent to info@srs.org
Return to TopICD-10: What does it mean for you?
ICD-10: What does it mean for you?
September 2012 Newsletter: R. Dale Blasier, MD
ICD-9-CM and ICD-9-PCS (International Statistical Classification of Diseases and other Health Problems) have been the standard code sets used for reporting diagnoses and inpatient procedures in the United States since 1979. This 34 year old system was implemented by the World Health Organization (WHO) for the purpose of reporting morbidity and mortality information for vital health statistic tracking and research. This classification system is no longer capable of keeping up with the advances in medical practice, treatment, health information needs, or payment processes.
For practices throughout the United States this means change from the current 14,000 code diagnosis system (ICD-9-CM) to a new 68,000 diagnosis code system (ICD-10-CM). The current ICD-9 system can no longer accommodate new diagnoses of medical conditions or hospital inpatient procedures nor does it sufficiently specify disease etiology, anatomical site, and severity. ICD-9 also does not accurately reflect advances in medical technology, treatment or knowledge; it has limited ability to measure health care services or conduct public health surveillance; and it cannot accurately measure quality of care, outcomes, safety, and security.
The new system has five to seven characters and will permit these codes to be placed within their correct category while allowing more specificity to accommodate subcategories of diseases and health problems. Laterality will also be addressed with the new system.
Due to expanded character length in ICD-10, system upgrades to medical records will require a change from Version 4010 of the HIPAA electronics administrative transactions to Version 5010. Implementation will take great preparation, thorough planning, training, time and financial resources. Implementation will affect all areas of practice and work staff. All forms that include diagnosis codes, particularly superbills and encounter forms, will need to be updated. All staff will need to be educated. Starting implementation early will help to make this process less disruptive and will provide for a more effective and efficient transition.
Return to TopCoding for Deformity Combined with Degenerative Stenosis: A Case Example
Coding for Deformity Combined with Degenerative Stenosis: A Case Example
March 2012 Newsletter: Patrick J. Cahill, MD
Spinal deformity surgery and spinal surgery for degenerative conditions are not mutually exclusive fields. If a Venn diagram were used to describe the two fields, there would be significant overlap. Even on the level of a single patient, degenerative and deforming processes may be contributing to pathology. ICD-9, however, attempts to stratify and codify surgical procedures into one category or the other. This can be confusing for surgeons and those coding their procedures. This article will attempt to provide some guidance in surgical coding in cases where the distinction between degenerative and deformity conditions is blurry.
The overriding principle should be correct coding rather than maximizing reimbursement. The surgeon should decide the primary indication(s) for performing a specific procedure and select the code or codes for that procedure. For example, if a surgeon removes the facet joints and ligamentum flavum at a lumbar level on which she or he is operating to increase flexibility and improve correction, then the procedure should be coded as a single column posterior osteotomy (22214). However, if the structures were removed for bilateral foraminal stenosis and/or neural compression then the procedure should be billed as a decompressive procedure (63047).
The case below illustrates some of the principles of correct coding where a combination of degenerative stenosis and deformity exist. The patient is a middle aged gentleman with a degenerative spondylolisthesis fused at L4-5, then later extended to L3-4, who developed sagittal imbalance after discitis destroyed the L2-3 disc space. The pre-operational CT-myelogram shows severe stenosis at L2-3 and moderate stenosis at L1-2. The surgeon performed an L4 pedicle subtraction osteotomy (PSO), L1-pelvis posterior instrumented spinal fusion, with laminectomies from L1-3. The patient had pathology related to deformity and degenerative issues-focal kyphosis resulting in global sagittal imbalance as well as symptomatic stenosis. The surgeon performed a surgery to address these issues. The PSO and instrumentation treated the deformity and the decompression treated the stenosis.
Thus, the surgery combines several individual components: arthrodesis, removal of instrumentation, insertion of instrumentation (to pelvis), decompression, osteotomy, and insertions of allograft and locally obtained autograft.
The deformity correction is addressed by several codes including 22800 (posterior arthrodesis for deformity up to six segments), 22207 (three column lumbar osteotomy), 22842 (three to six segment lumbar instrumentation), 22848 (pelvic instrumentation), 20936 (locally harvested autograft), and 20930 (allograft). The surgeon selected these codes based on the indications and goals of the specific procedures.
Note that the arthrodesis codes are stand-alone codes, which mean that they are 90-day global codes which can be coded and billed in isolation and include pre-operative evaluation and post-operative care. Several of the other codes, (instrumentation and allograft) are add-on codes and cannot be billed in isolation. Interestingly, while it is appropriate to bill for the bone graft codes 20930 and 20936, neither is assigned any work value by Medicare, although some private payers may reimburse for this procedure. Note that even though the original instrumentation is removed, it is not appropriate to code for this procedure as it is presumed by payers to be included in the insertion procedure, according to CPT rules. This is supported by an update for CPT coding issued in February 2012 by the American Academy of Orthopaedic Surgeons (AAOS) stating:
"Guideline changes also address removal of instrumentation and insertion of new instrumentation, including all or part of the previously instrumented segments as well as reinsertion at the same level. In years past, the surgeon reported the removal of old hardware (22850,22852,22855) and also reported the placement of new hardware when the procedures were performed at different levels.
Beginning in 2012, if a new surgeon removes instrumentation at L3-L4 and inserts new instrumentation from L1 through L5, only the new instrumentation codes should be reported---not codes for both the removal of the old instrumentation and the insertion of the new instrumentation. If the surgeon removes old instrumentation."
Instrumentation to the pelvis should only be coded if the instrumentation extends to the ilium. Instrumentation to the sacrum alone does not merit use of this code. The osteotomy code 22207 is also a stand-alone code and is actually valued more than the arthrodesis code 22800, so would be listed first and the 22800 would be listed subsequently and appended by the -51 modifier so as to avoid billing again for pre- and post-operational work.
The decompression codes 63047 (lumbar laminectomy and facetectomy with foraminal decompression) and 63048 (additional level) were selected to describe the laminectomy procedures since the primary indication was decompression of neurologic structures and not malalignment or instability. 63047 is a stand-alone code, but since it is done in conjunction with the arthrodesis and osteotomy procedures and is valued less, it is appended with the -51 modifier to avoid billing again for pre- and post-op work. 63048 is an add-on code and needs no modifier.
Each of the stand-alone codes must be supported by a diagnosis from ICD-9. The arthrodesis and the osteotomy codes can be justified by 737.10, Kyphosis (acquired) (postural), or 737.41 - Kyphosis. The decompression codes can be justified by 724.02, spinal stenosis, lumbar region without neurogenic claudication or 724.03 with claudication.
Unlike surgical procedures performed in other regions of the body, spine surgeries often require several codes to properly describe what is actually done. A good working knowledge of the codes and their proper interactions is needed to accurate document and bill for the performed services.
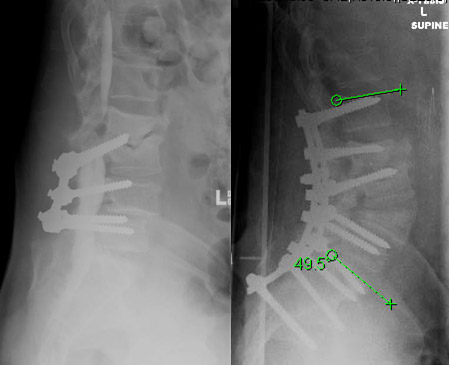
Pre- (left) and Post- (right) op images of an adult male who underwent a revision surgery for sagittal imbalance and stenosis.
Thanks to Anthony Rinella, MD and Wendy Benefeldt of Illinois Spine & Scoliosis Center and Jacob Buchowski, MD of Washington University, in assisting with the preparation of this article.
Return to TopCoding for Growing Rod Surgery
Coding for Growing Rod Surgery
September 2011 Newsletter: Jeffrey B. Neustadt, MD
The Coding Committee has been asked to provide the membership with advice and examples to help understand the complexity of coding and reimbursement issues specific to spine and spinal deformity surgeons. Every effort has been made to be accurate and adhere to the ICD-9 coding conventions and guidelines as well as the CPT rules. However there may be unintended discrepancies or differences of opinion. With that in mind, these articles are not intended to provide legal advice to surgeons and their staffs. The information given by the committee should not be relied upon as an official interpretation of the AMA CPT® code book. The American Medical Association (AMA) is the only entity which can give an official and binding interpretation of the AMA CPT® code book, and should be contacted directly if an official comment is needed or desired. For more information contact the AMA CPT® Network at www.cptnetwork.com. It is our every intention that the articles we prepare for this year’s newsletters are helpful and useful to all members of the SRS and their staffs. - Jeffrey B. Neustadt, MD, Chairman, Coding Committee
Growing rod surgery does not have specific or accurate CPT codes assigned. The initial surgery includes segmental instrumentation, limited fusions, as well as bone grafts. Lengthening surgery may or may not include a revision to the instrumentation. The conversion of a growing rod construct to a final posterior spine fusion with instrumentation involves removal of segmental instrumentation, more fusion, insertion of different instrumentation, bone grafts, and possibly Ponte or Smith-Petersen osteotomies. With this potpourri of procedures, accurate CPT coding becomes challenging. Therefore the Coding Committee felt a discussion of this topic would be of interest given the growing incidence of this type of spinal deformity surgery.
The following scenario will illustrate the use of CPT codes which may be considered appropriate for use in growing rod-related surgical procedures:
An ambulatory, five year old girl with syndromic scoliosis which has progressed to 90 degrees and includes significant pelvic obliquity undergoes growing rod instrumentation from T4 to the pelvis. Pedicle screws are placed bilaterally at T4 and T5 as well as at L5 and S1 along with bilateral iliac screws. Iliac bolt connectors are used to connect the iliac screws to two rods (actually four rods: two on each side connected by growing rod connectors) extending from T4 to the sacrum. Local bone and allograft demineralized bone matrix soaked in bone marrow aspirate is used as bone graft to fuse T4 to T5 and L5 to S1. The following CPT codes would be appropriate:
- 22800 - Arthrodesis, posterior, for spinal deformity, up to 6 vertebral segments
- 22844 - Posterior segmental instrumentation (e.g., pedicle fixation, dual rods); 13 or more vertebral segments
- 22848 - Pelvic fixation (attachment of caudal end of instrumentation to pelvic Bony structures) other than sacrum
- 38220 - Bone marrow aspirate for the purpose of bone grafting
Note that 22844 and 22848 are Modifier 51 Exempt. 38220 is NOT modifier 51 Exempt.
Coding experts advise use of the following codes as well, although they have no relative value units assigned and therefore do not result in additional reimbursement:
- 20930 - Allograft for spine surgery only; morselized
- 20937 - Autograft for spine surgery only (includes harvesting the graft); local (e.g., ribs, spinous process, or laminar fragments) obtained from the same incision.
Six months later, the child undergoes a lengthening of the growing rod instrumentation. There is no accurate CPT code for this procedure. Two possible codes may be considered:
- 22849 - Reinsertion of spinal fixation device
- 22899 - Unlisted procedure, spine
While the latter code may seem more appropriate, it is problematic for most insurance companies as it requires a detailed explanation for why it is being used and still may be denied.
Six years later, the child undergoes a conversion to a full posterior spine fusion with instrumentation. Her growing rods are removed; the iliac screws and the screws at T4, T5, L5, and S1 are converted to larger screws which will accommodate 5.5 mm rods rather than 4.5 mm rods; more screws are placed at multiple segments from T5 to L4; 5 Ponte osteotomies are performed from T10 to L3 to improve correction of the significant thoracic hypokyphosis, and two Smith-Petersen osteotomies are performed at T6 and T7 where autofusion occurred over the years; a fusion from T5 to L5 is performed using local bone graft, allograft, and bone marrow aspirate. The following CPT codes would be utilized:
- 22852 - Removal of posterior segmental instrumentation
- 22802 - Arthrodesis, posterior, for spinal deformity; 7 to 12 vertebral segments
- 22844 - Posterior segmental instrumentation; 13 or more vertebral segments
- 22848 - Pelvic instrumentation
- 22214 - Osteotomy of spine, posterior or posterolateral approach, one vertebral Segment; lumbar
- 22216 - Osteotomy of spine, posterior or posterolateral approach, one vertebral Segment; each additional vertebral segment X 6
- 38220 - Bone marrow aspirate for bone grafting purposes
- 20930 - Allograft for spine surgery only; morselized
- 20937 - Autograft for spine surgery only (includes harvesting the graft); local
Note that although the segmental instrumentation spans more than 12 levels or segments, the fusion only spans 12 because the patient already underwent fusion of T4 to T5 and L5 to S1, leaving only T5 to L5 to be fused. Therefore CPT code 22802 is utilized rather than 22804 which would be for arthrodesis of 13 or more vertebral segments.
Also note that if no new levels were instrumented and the surgeon merely replaced the original screws with ones accommodating larger rods, one would not use 22844 and 22848 but instead would use 22849 - reinsertion of spinal fixation device.
Codes 22852, 22214, 22216, 22849 and 38220 are not Modifier 51 Exempt, while codes 222802 (the primary code here because it has the highest number of RVU's assigned), 22844, and 22848 are Modifier 51 Exempt.
Correct coding is important both for correct reimbursement as well as correct documentation of surgical procedures performed. As one can see with the scenario of growing rod instrumentation, it is not always possible to find codes which accurately reflect what was done. In such situations, consultation with coding experts may be helpful. Appeals of denied codes may also be necessary. As always, accurate dictated documentation of performed procedures is mandatory.
Return to TopUpdate on Coding for Correction of Spinal Deformity
Update on Coding for Correction of Spinal Deformity
March 2011 Newsletter: Jeffrey B. Neustadt, MD and R. Dale Blasier, MD
The Coding Committee has been asked to provide the membership with advice and examples to help understand the complexity of coding and reimbursement issues specific to spine and spinal deformity surgeons. Every effort has been made to be accurate and adhere to the ICD-9 coding conventions and guidelines as well as the CPT rules. However there may be unintended discrepancies or differences of opinion. With that in mind, these articles are not intended to provide legal advice to surgeons and their staffs. The information given by the committee should not be relied upon as an official interpretation of the AMA CPT® code book. The American Medical Association (AMA) is the only entity which can give an official and binding interpretation of the AMA CPT® code book, and should be contacted directly if an official comment is needed or desired. For more information contact the AMA CPT® Network at www.cptnetwork.com. It is our every intention that the articles we prepare for this year's newsletters are helpful and useful to all members of the SRS and their staffs. - Jeffrey B. Neustadt, MD, Chair, Coding Committee
Correct procedural coding for correction of spinal deformity involves several unique issues. The common relevant issues include appropriate use of fusion levels, base codes, add-ons and modifiers. This article discusses several deformity correction scenarios and provides specific examples for their accurate coding.
Space does not allow for inclusion of all deformity correction coding issues, for example, video-assisted thorascopic surgery, vertical expandable prosthetic titanium rib, growing rods, anterior growth tethering surgery, kyphectomy, kyphoplasty, vertebroplasty and vertebral resection. These will be covered in future newsletters.
Determining Fusion Levels
In coding deformity correction, the number of segments involved in the surgery must be determined. The number of levels (2 segments = 1 level; total levels = total segments-1) determines the codes which will be used for the arthrodesis. The instrumentation code is based on the number of segments spanned. Typically these are the same but they may not be in some cases, e.g. posterior spinal fusion with instrumentation from T4 to L4. This would be coded as fusing 12 levels but instrumenting 13 segments. More on this later!
Base Codes and Add-Ons
All deformity corrections are described by one or more codes. Every surgical episode must have a base code, i.e. a code which can stand on its own. For spine, these include the codes for arthrodesis, osteotomy, hardware removal and reinsertion. Several common procedures such as instrumentation, bone grafting, insertion of cages, fixation to the pelvis and thoracoplasty are add-on codes which can never be reported by themselves. These must be reported in addition a base code.
Modifiers
Base codes are generally billed without modifiers and are expected to be reimbursed by payers at 100% of the usual rate. The preop evaluation, postop care and subsequent patient visits are presumed to be reimbursed by the base code. Add-on codes are valued based upon intraoperative work only and do not include reimbursement for preop evaluation or postop care. For this reason, they do not need multiple procedure modifiers and are not discounted by payers.
If multiple base codes are performed during the same procedure, the largest base code is generally billed first and is not discounted by the payer. Lesser base codes are billed subsequently and are appended by the 51 modifier. Because these codes are valued to include pre and postop care which is redundant with the primary base code, the 51 modifier enables the payer to discount these codes to prevent multiple reimbursements for perioperative care. When using the osteotomy codes at multiple levels, some payers require the use of modifier 59 (distinct procedural service) to indicate additional separate levels and other payers require modifier 76 (repeat procedure by same physician).
Base Codes: Descriptions
Procedures which can be done by themselves and are valued to include pre and postoperative work are indicated with base codes. These include arthrodesis (fusion), osteotomy and hardware removal or reinsertion:
- Arthrodesis Codes
Posterior:- 22800 Arthrodesis, posterior, for spinal deformity, with or without cast; up to 6 vertebral segments (levels)
- 22802 Arthrodesis, same; 7 to 12 vertebral segments (levels)
- 22804 Arthrodesis, same; 13 or more vertebral segments (levels)
- 22806 Arthrodesis, anterior, for spinal deformity, with or without cast; 2 to 3 vertebral segments (levels)
- 22808 Arthrodesis, anterior, same; 4 to 7 vertebral segments (levels)
- 22812 Arthrodesis, anterior, same; 8 or more vertebral segments (levels)
- Osteotomy Codes
- 22206 Osteotomy of spine, posterior or posterolateral approach, three columns, one vertebral segment (eg, pedicle/vertebral body subtraction); thoracic
- 22207 Osteotomy of spine, posterior or posterolateral approach, three columns, one vertebral segment (eg, pedicle/vertebral body subtraction); lumbar
- 22212 Osteotomy of spine, posterior or posterolateral approach, one vertebral segment; thoracic
- 22214 Osteotomy of spine, posterior or posterolateral approach, one vertebral segment; lumbar
- Hardware Manipulation
- 22849 Reinsertion of spinal fixation device
- 22250 Removal of posterior nonsegmental instrumentation (eg, Harrington rod)
- 22852 Removal of posterior segmental instrumentation
- 22855 Removal of anterior instrumentation
Add-on Codes: Descriptions
Add-on services (those with a ZZZ global period) contemplate services which are only intraoperative service. No pre or postop care is included. These always must be billed in addition to a base code. Note that instrumentation can never be billed alone. It must always be performed in association with a base code which complicates coding for growing rod procedures.
- Instrumentation Codes:
Anterior:- 22845 Anterior instrumentation; 2 to 3 vertebral segments
- 22846 Anterior instrumentation; 4 to 7 vertebral segments
- 22847 Anterior instrumentation; 8 or more vertebral segments
- 22840 Posterior non-segmental instrumentation (eg, Harrington rod technique, pedicle fixation across one interspace, atlantoaxial transarticular screw fixation, sublaminar wiring at C1, facet screw fixation)
- 22841 Internal spinal fixation by wiring of spinous processes
- 22842 Posterior segmental instrumentation (eg, pedicle fixation, dual rods with multiple hooks and sublaminar wires); 3 to 6 vertebral segments
- 22843 same; 7 to 12 vertebral segments
- 22844 same; 13 or more vertebral segments
- Add-on Osteotomy:
Three-column:- 22208 Osteotomy of spine, posterior or posterolateral approach, three columns, one vertebral segment (eg, pedicle/vertebral body subtraction); each additional vertebral segment
- 22216 Osteotomy of spine, posterior or posterolateral approach, one vertebral segment; each additional vertebral segment
- Bone Grafting
Bone graft codes represent the harvest of the graft only. Reimbursement for implantation of the graft is included in the arthrodesis code. Note that 20930 and 20936 describe procedures that have been assigned a zero RVU value. 20930 Allograft, morselized, or placement of osteopromotive material, for spine surgery only. Note that this code descriptor has been modified for 2011 to include "osteopromotive material".
- 20931 Allograft for spine surgery only; structural
- 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process, or laminar fragments) obtained from same incision
- 20937 Autograft for spine surgery only (includes harvesting the graft); morselized (through separate skin or fascial incision)
- 20938 Autograft for spine surgery only (includes harvesting the graft); structural, bicortical or tricortical (through separate skin or fascial incision)
- Instrumentation to Pelvis
- 22848 Pelvic fixation (attachment of caudal end of instrumentation to pelvic bony structures) other than sacrum
- Thoracoplasty
No code describes this procedure well. The following have been reported with success:
- 32905 Thoracoplasty, Schede type or extrapleural (all stages)
- 22899 Unlisted procedure, spine
- Insertion of cages
Note that insertion of machined allograft is specifically not listed in this code descriptor:- 22851 Application of intervertebral biomechanical device(s) (eg, synthetic cage[s], methylmethacrylate) to vertebral defect or interspace. Note that this code descriptor has been modified for 2011 to eliminate "threaded bone dowel[s]".
Other Adjunctive Procedures
Generally, supervision and interpretation of imaging for spine surgery - even for insertion of pedicle screws - is considered part of the procedure and should not be billed separately. Preparation and insertion of centrifuged blood products for deformity surgery is not reimbursable.
Examples of Surgical Coding
Scenario 1: Posterior Spinal Fusion for Kyphosis
This scenario describes a patient with kyphosis with an apex at T9. Instrumentation and fusion are performed from T2 to L2 (13 vertebrae, 12 segments or levels). Ponte or Smith-Petersen osteotomies are performed at T8-9, T9-10 and T10-11. Fragments excised at osteotomy are added to the fusion mass as bone graft. Additional graft is taken through a separate incision from the iliac crest.
For this procedure, the base code is: 22802 Arthrodesis, posterior, for spinal deformity, with or without cast; 7 to 12 vertebral segments. The osteotomies could also be base codes because they are 90-day global codes, but the arthrodesis code has a higher RVU value.
The first osteotomy should be billed as: 22212 Osteotomy of spine, posterior or posterolateral approach, one vertebral segment; thoracic and should be appended with a 51 modifier because it is a 90-day global code.
The second and third osteotomies should be billed as: 22216 Osteotomy of spine, posterior or posterolateral approach, one vertebral segment; each additional vertebral segment. This is an add-on code and does not require a modifier.
The instrumentation should be billed as: 22844 Posterior segmental instrumentation; 13 or more vertebral segments. This is an add-on code and does not require a modifier.
The iliac bone graft should be billed as: 20937 Autograft for spine surgery only (includes harvesting the graft); morselized (through separate skin or fascial incision). This is an add-on code which does not require a modifier. Note that bone graft codes assign value to the harvest and not the implantation.
The bone graft taken as fragments from the osteotomy should be billed as: 20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process, or laminar fragments) obtained from same incision. While this is billable, no work value is assigned to this code.
Scenario 2: Anterior Spinal Fusion for Scoliosis:
This scenario describes a patient with scoliosis with an apex at L1. The spine is approached by a right thoracolumbotomy. Instrumentation and fusion are performed from T11 to L3 (five vertebrae, four segments or levels). Fragments of the eleventh rib excised at thoracotomy are placed in the intervertebral spaces as bone graft. Cages are placed at the two lowest intervertebral spaces to maintain lumbar lordosis. During closure, a chest tube is placed.
The base code is:
22808 Arthrodesis, anterior, for spinal deformity, with or without cast; four to seven vertebral segments. The surgical approach is not separately billable. If another surgeon makes the approach for the spine surgeon, then spine and approach surgeon become co-surgeons for the base code which is appended by modifier 62. The base code includes preparing the disc spaces and insertion of bone graft.
The instrumentation code is:
22846 Anterior instrumentation; 4 to 7 vertebral segments) and includes any rod rotation, compression or distraction used to correct the deformity. No modifier is needed as this is an add-on code.
The bone graft is billed as:
20936 Autograft for spine surgery only (includes harvesting the graft); local (eg, ribs, spinous process, or laminar fragments) obtained from same incision No modifier is needed as this is an add-on code. Note that the code has zero value.
The insertion of cages is billed as two episodes of:
22851 Application of intervertebral biomechanical device(s) (eg, synthetic cage(s), methylmethacrylate) to vertebral defect or interspace. No modifier is needed as this is an add-on code. The insertion, maintenance, and removal of the chest tube are included in the approach and are not separately billable.
Scenario 3: Posterior Spinal Fusion for Neuromuscular Scoliosis
This scenario describes a patient with a collapsing scoliosis of the whole spine. Instrumentation and fusion are performed from T2 to the sacrum (17 vertebrae, 16 segments or levels). Multiple pedicle screws, hooks and sublaminar wires are placed to secure the rods. Instrumentation stops at the sacrum and does not extend to the iliac wings. The iliac wings are small, osteoporotic and not considered a good source of graft, so allograft and a centrifuged blood product are placed to encourage fusion after the facet joints are excised.
The base code is: 22804 Arthrodesis, posterior, for spinal deformity, with or without cast; 13 or more vertebral segments.
The instrumentation code is:
22844 Posterior segmental instrumentation (eg, pedicle fixation, dual rods with multiple hooks and sublaminar wires); 13 or more vertebral segments).
If the instrumentation had extended to the ilia, it would have been appropriate to add: 22848 Pelvic fixation (attachment of caudal end of instrumentation to pelvic bony structures) other than sacrum.
Placement of allograft is described by:
20930 Allograft, morselized, or placement of osteopromotive material, for spine surgery only
Placement of a centrifuged blood product is not covered by any code.
Return to TopCommon Coding Scenarios
The Coding Committee has been asked to provide the membership with advice and examples to help understand the complexity of coding and reimbursement issues specific to spine and spinal deformity surgeons. Every effort has been made to be accurate and adhere to the ICD-9 coding conventions and guidelines as well as the CPT rules. However there may be unintended discrepancies or differences of opinion. With that in mind, these coding scenarios are not intended to provide legal advice to surgeons and their staffs. The information given by the committee should not be relied upon as an official interpretation of the AMA CPT® code book. The American Medical Association (AMA) is the only entity which can give an official and binding interpretation of the AMA CPT® code book, and should be contacted directly if an official comment is needed or desired. For more information contact the AMA CPT® Network at www.cptnetwork.com.
- Early Onset Scoliosis (EOS) Scenarios
- Adolescent Idiopathic Scoliosis Scenarios
- Adult Scoliosis Scenarios
Early Onset Scoliosis (EOS) Scenarios
1. 7-year-old male with early onset scoliosis is treated with growing rod instrumentation that spans from T3-L4. The procedure entails use of pedicle screws with associated fusions at the cranial (T3-4) and caudal terminus (L3-4) of the construct, and use of morselized allograft at the T3-4 and L3-4 fusion sites. Two possible coding scenarios could be considered. The first scenario is most accurate as the deformity fusion codes best match the primary (deformity) diagnosis.
| 22800 | fusion deformity (<6 segments) |
| 22844 | growing rod instrumentation (>13 segments) |
| 20930 | morselized allograft |
| 22610 | fusion T3/4 |
| 22614 | fusion L3/4 each additional segment |
| 22844 | growing rod instrumentation (>13 segments) |
| 20930 | morselized allograft |
2. Expansion of the above growing rod construct. There is no accurate CPT code for this procedure, but two possible codes are most commonly used.
| 22849 | Reinsertion of spine instrumentation |
| 22899 | Unlisted procedure, spine |
We have listed the most common codes used for this procedure based on a previous SRS survey (Blasier SRS newsletter December, 2012.) The unlisted code (22899) is appropriate if there is no existing code which adequately describes the procedure. However, a letter documenting the details of the procedure, and why it is being used, is required. Currently, some SRS members are replacing this lengthening procedure with MAGEC rods in the office setting and therefore use E+M, not CPT codes.
3. Revision of the above growing rod construct due to rod fractures, requiring replacement of a new rod but no extension of the instrumented levels.
| 22849 | Removal of broken rods and reinsertion of new rods= reinsertion of spinal fixation/instrumentation |
CPT rule explains that “22849 should not be reported in conjunction with 22850, 22852, and 22855 at the same spinal levels.” The reinsertion code 22849 incudes the work for removal of instrumentation as well as the reinsertion (see Blasier SRS newsletter September 2013.)
4. Revision of the above growing rod construct due proximal junctional kyphosis requiring proximal extension of the construct to T2 with associated use of hooks at T2, fusion of T2-3, use of morselized allograft at the T2-3 fusion site, and implantation of longer rods bilaterally at the proximal section of the construct that extend from the T2 segment to growing rod lengthening segment (tandem connector).
| 22610 | fusion T2/3 posterior arthrodesis thoracic single level |
| 22840 | posterior nonsegmental instrumentation |
| 20930 | use of morselized allograft |
CMS National Correct Coding Initiative (NCCI) Mutually Exclusive Group edits do not allow for simultaneous use of 22840 and 22849. Since fusion and instrumentation is extended to a new level, use the appropriate instrumentation codes 22840-22848. Depending on the details of the procedure and accompanying documentation non segmental instrumentation (22840) and segmental instrumentation (22842) are possibilities.
5. 7-year-old male history of progressive early onset scoliosis due to cerebral palsy that is treated with a VEPTR device that extends from T2-pelvis, utilizing rib fixation at the cranial terminus of the construct and iliac screws at the caudal terminus of the construct. No associated bony fusion performed during the procedure.
| 22844 | VEPTR spanning T2-Pelvis |
| 22848 | Pelvic fixation with iliac screws, other than sacrum |
| 22899 | Unlisted procedure, spine |
To date, there is no code which accurately describes this coding scenario. Although the first code combination is used by SRS members (see Blasier SRS Newsletter, December 2012) it is problematic as both 22844 and 22848 are add-on codes that require a base code (see Update on Coding, SRS newsletter March 2011). If unlisted code (22899) is used, a letter documenting the details of the procedure, and why it is being used is required.
6. 3-year-old male treated with a cast (Risser, Mehta, elongation-derotation-flexion cast, etc.) for progressive early onset scoliosis.
| 29010 | = | general procedure on the musculoskeletal system | = | Casting for early onset scoliosis |
This a difficult coding scenario. Multiple codes are available for coding for a scoliosis cast, however no consensus exists for this procedure.
Frequently Asked Questions
To ask a question, please visit this form.
There are 141,000 codes in ICD-10. Do you have a cheat sheet?
- Download the pdf cheat sheet (pdf)
- For more information on ICD-10, feel free to browse the Centers for Medicare and Medicaid Services site, here
Tell me about coding for Autograft.
CPT code 20936 reads "Autograft for spine surgery only [includes harvesting the graft]; local [eg. ribs, spinous process, or laminar fragments] obtained from the same incision". The SRS agrees that local bone harvested from the spinal incision and within the area already being dissected to prepare for fusion is incidental to the posterior fusion codes CPT 22800-22804. This would include bone fragments from the posterior elements of the spine: laminar fragments, spinous processes and facets and perhaps rib heads or small fragments of the ribs obtained from the spinal dissection as it extends to the tip of the transverse processes. Surgeons would all agree that harvesting of ribs is an entirely different and independent procedure that falls under the code of 20937, " Autograft for spine surgery only: morselized through separate skin or fascial incision". Although the major spine incision may be used, another fascial incision is required and surgeons often use another parallel longitudinal incision centered over the rib hump. Even if the rib harvesting is through the main spinal incision, it requires a separate fascial incision, considerable dissection out laterally over the ribs, and a lengthy procedure to subperiosteally expose multiple ribs and remove them from the chest. It requires significant time and expertise, but certainly may be the surgeon's choice for the appropriate source of autologous graft material in order to obtain adequate amounts of autograft, to correct the rib hump deformity, and to allow further correction of the spinal deformity. (HH Steel, "Rib Resecton and Spine Fusion in Correction of Convex Deformity in Scoliosis" JBJS(A), 1983 Sept, 65(7) pp: 920-925. DC Mann, CL Nash Jr., MR Wilham, RH Brown, "Evaluation of the Role of Concave Rib Osteotomies in the Correction of Thoracic Scoliosis", Spine 1989, May, 14(5) pp:491-495.) When rib autograft is being harvested to serve as the primary graft material, that is another situation entirely than using local available bone. As above, harvesting of multiple lengthy segments of ribs includes not only extensive additional dissection and surgical knowledge and skill but also significant time in then preparing the rib segments into strips appropriate for graft material. This is not an incidental procedure to the main posterior arthrodesis codes 22800-22804. It is an additional procedure taking significant time, additional risk, additional blood loss and requires specialized knowledge and skill on the surgeon's part. It is done to obtain autograft by those surgeons who wish to use the patient's own bone and as an alternative to harvesting the iliac crest for autograft. Clearly CPT code 20937 would be the appropriate code in this case, not CPT 20936.
